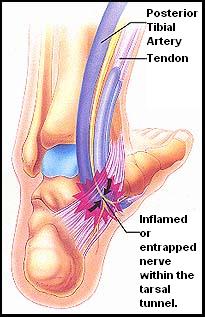
Posterior Tarsal Tunnel Syndrome is a painful problem in the foot that occurs due to compression of the tibial nerve. The tibial nerve travels down the back of the leg and through the posterior tarsal tunnel. The posterior tarsal tunnel is a space that lies on the inside of the ankle. The bones at that spot are covered by a thick ligament called a retinaculum that protects and maintains the nerves, arteries and veins that run through the tunnel. Compression of the nerves that run through the posterior tarsal tunnel causes pain, numbness and tingling similar to carpal tunnel syndrome. The symptoms are felt on the inside of the ankle or on the bottom of the foot. The patient may also have weakness of the toes and instability of the foot muscles. The pain occurs more often at night than during the day. The symptoms are brought on by trauma or overuse, such as exercise, walking or bicycling. Patients at risk for posterior tarsal tunnel syndrome include those with fractures, diabetes, rheumatoid arthritis or an abnormal structure that occupies the space such as a ganglion cyst or bone spur. An MRI is useful to look for causes of posterior tarsal tunnel syndrome such as fractures or cysts. An EMG is a nerve test that is useful to distinguish posterior tarsal tunnel syndrome from other causes of pain such as diabetic neuropathy or a herniated disc causing lumbar radiculopathy. Mild cases often respond to conservative modalities such as rest, heat, ice, physical therapy and non-steroidal anti-inflammatory medications. Injection of the area with a corticosteroid can decrease the irritation and inflammation of the nerve and may reduce the pain allowing the other modalities of treatment to be more successful. Pain and symptoms that are refractory to conservative treatment may require surgery to release the nerve from its entrapment.